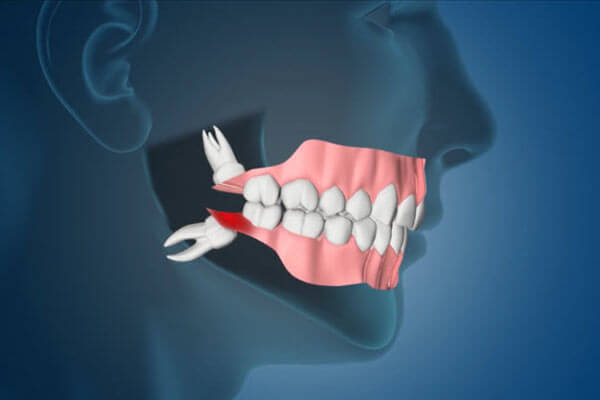
Wisdom teeth, also known as third molars, are the last teeth to erupt in your mouth. This generally occurs between the ages of 17 and 25, a time of life that has been called the “Age of Wisdom.”
Anthropologists note that the rough diet of early humans resulted in the excessive wear of their teeth. Normal drifting of the teeth to compensate for this wear ensured that space was available for most wisdom teeth to erupt by adolescence. The modern diet, which is much softer, and the popularity of orthodontic tooth straightening procedures produce a fuller dental arch, which quite commonly doesn’t leave room for the wisdom teeth to erupt, thereby setting the stage for problems when the final four molars enter the mouth.
WHAT ARE IMPACTED WISDOM TEETH?
Complications such as infection (fig. a) , damage to adjacent teeth (fig. b) and the formation of cysts (fig. c) may arise from impacted teeth.
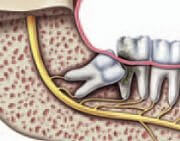
(a) Infection
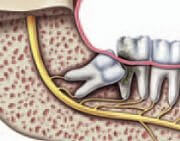
(b) Crowding, damage
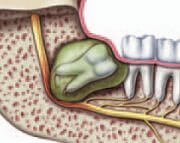
(c) Cyst
A tooth becomes impacted when there is a lack of space in the dental arch and its growth and eruption are prevented by overlying gum, bone or another tooth.
HOW SERIOUS ARE IMPACTED WISDOM TEETH?
Impacted teeth can be painful and lead to infection.They may also crowd or damage adjacent teeth or roots.
More serious problems may occur if the sac surrounding the impacted tooth becomes filled with fluid and enlarges to form a cyst. As the cyst grows, it may hollow out the jaw and permanently damage adjacent teeth, the surrounding bone and nerves. It is rare, but if a cyst is not treated, a tumor may develop from its walls and a more serious surgical procedure may be required to remove it.
Despite the considerable concern regarding impacted third molars, a recent study sponsored by the American Association of Oral and Maxillofacial Surgeons (AAOMS) and the Oral and Maxillofacial Surgery Foundation (OMSF) finds that third molars which have broken through the tissue and erupted into the mouth in a normal, upright position may be as prone to disease as those third molars that remain impacted.
MUST THE TOOTH COME OUT IF IT HASN’T CAUSED ANY PROBLEMS YET?
Not all problems related to third molars are painful or visible. Damage can occur without your being aware of it.
- As wisdom teeth grow, their roots become longer
- The teeth become more difficult to remove and complications become more likely
- As patients age, impacted wisdom teeth are more likely to cause problems
No one can predict when third molar complications will occur, but when they do, the circumstances can be much more painful and the teeth more difficult to treat. It is estimated that about 85% of third molars will eventually need to be removed.
WHEN SHOULD I HAVE MY WISDOM TEETH REMOVED?
Wisdom teeth are easier to remove when the patient is younger. Since their roots are not completely formed, the surrounding bone is softer and there is less chance of damaging nearby nerves or other structures. Removal of wisdom teeth at a later age becomes more complicated, as the roots have fully developed (may involve the nerve), and the jawbone is denser.
It isn’t wise to wait until your wisdom teeth start to bother you. In general, earlier removal of wisdom teeth results in a less complicated healing process.The AAOMS/OMSF study strongly recommends that wisdom teeth be removed by the time the patient is a young adult in order to prevent future problems and to ensure optimal healing.The researchers found that older patients may be at greater risk for disease, including periodontitis, in the tissues surrounding the third molars and adjacent teeth. Periodontal infections, such as those observed in this study, may affect your general health.
WHAT HAPPENS DURING SURGERY?
At your consultation visit, your oral and maxillofacial surgeon will discuss with you what to expect. This is a good time to ask questions or express your concerns. It is especially important to let the doctor know about any illness you have and medications you are taking. It is also your best opportunity to discuss what type of anesthesia you will need.
The relative ease with which a wisdom tooth may be removed depends on several conditions, including the position of the tooth and root development. Impacted wisdom teeth may require a more involved surgical procedure.
Most wisdom tooth extractions are performed in the oral and maxillofacial surgery office under local anesthesia, intravenous sedation or general anesthesia. Your oral and maxillofacial surgeon will discuss the anesthetic option that is right for you.
WHAT HAPPENS AFTER SURGERY?
Following surgery, you may experience some swelling and mild discomfort, which are part of the normal healing process. Cold compresses with ice may help decrease the swelling and pain. Medication prescribed by your Oral and Maxillofacial Surgeon can help manage the pain and discomfort. You may be instructed to modify your diet following surgery and later progress to more normal foods.
WHAT CAN I EAT AFTER MY WISDOM TEETH REMOVAL?
While it is hard to eat for the first few days following wisdom teeth extraction, it is important not to skip meals and to stay well nourished to help maintain strength and heal faster. For the first day or two, it is best to eat mostly soft foods or liquids such as:
- Smoothies
- Yogurt
- Shakes
- Pureed foods
- Soups
- Pudding and Jello
- Popsicles
It is best to avoid drinking through a straw, as this could dislodge blood clots healing the sockets and cause dry sockets. You should also avoid eating the following:
- Extremely spicy foods, because this can cause irritation of the surgical site
- Drinking hot beverages for several days following surgery should be avoided, as this could dislodge blood clots that are helping the healing process.
- Stay away from foods that can get caught in the extraction socket like nuts, rice, seeds, and popcorn.
As the extraction areas start to heal, regular foods that require chewing can be slowly introduced back into the diet, depending on the comfort of the person.
POSSIBLE RISKS AND COMPLICATIONS AFTER WISDOM TEETH REMOVAL
Most wisdom teeth removals have a relatively uneventful postoperative recovery. The most common adverse occurrence of a wisdom tooth extraction is a dry socket, otherwise known alveolar osteitis. This condition is created when the blood clot in the surgical site becomes dislodged, leaving exposed bone and nerves. Once this occurs, the bone along the extraction socket becomes inflamed and painful. If it happens, a dry socket will typically develop between two and five days after the extraction and will produce a bad smell/taste in the mouth along with constant throbbing pain. If you suspect a dry socket, your surgeon should be contacted. This complication is easily treated and often resolves quickly with a packing medication or stimulation of a new blood clot. More serious complications are rare but can include:
- Injury to the adjacent inferior alveolar nerve for wisdom teeth on the bottom of the mouth (mandible)
- Sinus perforation for wisdom teeth on the top of the mouth (maxilla)
- Damage to adjacent teeth
- Prolonged numbness or altered sensation of the tongue, lip, or gum tissue (paresthesia)
- Problems with the temporomandibular joint as a result of trauma to the area.
The potential risks of wisdom teeth extraction should be reviewed with a dentist. If a wisdom tooth is deemed compromised, removal of the tooth or teeth in adolescence is advantageous to extracting the tooth in late adulthood. The extraction procedure and healing both become more difficult as the person gets older. Discussion with a dentist about the condition of the wisdom teeth and timeline for the extractions is important and will help minimize complications. To consider a wisdom tooth replacement or replace missing teeth after wisdom tooth removal should be discussed with the doctor first.
See Also: Dental Implant Surgery or Instructions For After Your Procedure